- Giuseppe Ruocco
- Review
Angioedema: a rare and potential fatal case
- 3/2019-Ottobre
- ISSN 2532-1285
- https://doi.org/10.23832/ITJEM.2019.031
Giuseppe Ruocco1, Alessio Faricciotti 2
- Dipartimento di emergenza e urgenza UOC Medicina e chirurgia di accettazione e d’urgenza ASST Rhodense – RHO (MI)
- Dipartimento Medicina UOC Oncoematologia ASST Rhodense – RHO (MI)
Introduction
Urticaria (localized and detected erythematous reaction of the skin) is a frequent cause of access in the departments of emergency medicine1,2. Angioedema (edema of the tissues deeper than the dermis or not) may be associated with urticaria, but in 10% of cases occurs alone. In most cases urticaria/angioedema have a pathogenesis mediated by histamine, more frequently secondary to the intake of drugs (especially Ace inhibitors and NSAIDs) or food3,4. Rare causes are non-immunological ones: physical ones (eg pressure, cold or sunlight urticaria) those from psychophysical stress and those from hereditary and non-hereditary protein deficiency (e.g. C1inhibitor)4,5,6.
Case Report
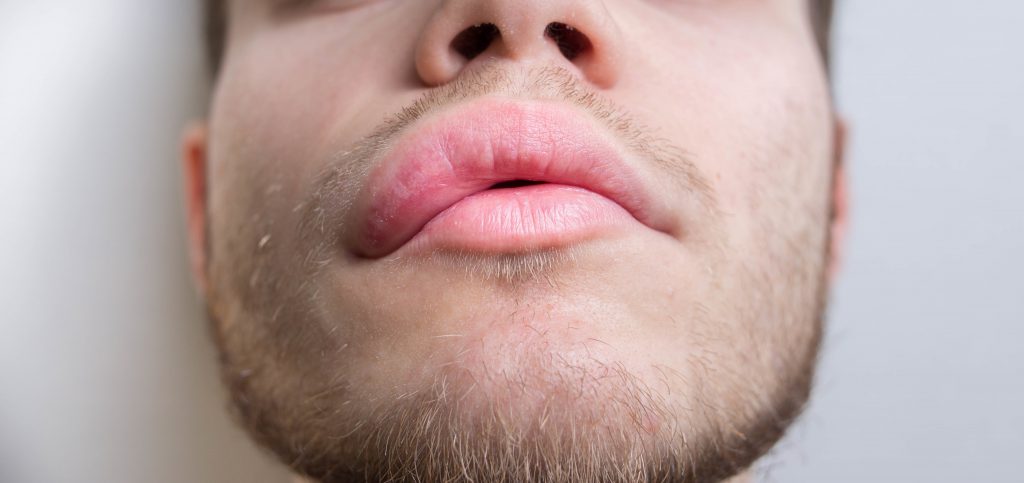
Mr. P.G. of 75 years arrived in the emergency department at 4.16 am for edema of the lips and tongue with paresthesias after intake the previous evening of strawberries and ham with dinner. The patient reported a history of type 2 diabetes mellitus, non-Hodgkin’s lymphoma and previous infiltrating bladder carcinoma. At the arrival the vital parameters were stable with SO2 98% HR 87 RR 18 and BP 140/80 mmHg.
The physical examination showed a macroglossia, edema of the soft palate (without edema of the uvula) and absence of bronchospasm. Therefore routine blood tests were performed and Methylprednisolone 80 mg iv, Chlorfenamine maleate 1 fl im, aerosol with Beclomethasone dipropionate A 1 fl + Salbutamol solfate 10 gtt were administered. After about 2 hours for reported worsening of the edema to the tongue proceeded to further cortisone therapy with Methylprednisolone 40 mg and subsequently with 500 mg of hydrocortisone. Prior reanimation evaluation was required with an additional indication of other 500 mg of hydrocortisone plus ranitdine 1fl and aerosol with adrenaline. At 7.45 am the patient became frankly agitated, pale, tachypnoic, and subsequently asphyxiated. So he was transported in the emergency room with the appearance of respiratory arrest and subsequently cardiac arrest.
Upon rapid resumption of circulation after cardiac massage, a difficult orotracheal intubation was performed with a cannula 6.5 by fast track for edematous glottal plane. He was then admitted to the ICU. The stay in ICU was regular. In suspect of acquired angioedema, dosage of C1 inhibitor, C3 and C4 was requested, which was below normal values. Therefore the patient was transferred to the oncohematology department and started a therapy with fresh frozen plasma and C1 inhibitor with progressive clinical improvement and discharge after 17 days.
Discussion
Acquired angioedema is a rare disease caused by a C1-inhibitor deficiency; this deficiency can be acquired when
1) Complement factors are consumed by neoplastic pathologies (eg LNH) or in immunocomplex diseases7,9.
2) There are autoantibodies directed against the C1 inhibitor (eg monoclonal gammopathy or
during autoimmune diseases such as LES and dermatomyositis). The prevalence of acquired angioedema is 1/50000; clinical presentation is usually in adulthood (over 40 years) and the triggers may be trauma (even mild) virosis, exposure to cold, pregnancy or ingestion of certain foods; Edema may affect the face, lips, tongue, uvula, and gastrointestinal tract with signs of intestinal obstruction. Not rarely, hereditary angioedema affects the larynx with edema of the glottis and death by asphyxiation in 25% of cases if orotracheal intubation is not readily performed. If the airways are involved, ensuring a patent airway has the highest priority; Adrenaline may provide transient benefit in acute attacks when the airways are involved while corticosteroids and antihistamines are not effective being this an edema not induced by histamine. Solvent treatment consists of the administration of the deficient C1 inhibitor factor.
In addition, some forms of angioedema mediated by bradykinin are efficiently treated with a beta2 receptor antagonist, icatibant, although its use in these cases is off label10. Therefore the required treatment varies depending on the pathological mechanism responsible for the increased vascular permeability (histamine/bradykinin).
Conclusions
Angioedema attacks, characterized by the transient swelling of the skin and mucosae, are a frequent cause of access to the emergency room8. Not being on an allergic basis, acquired angioedema it is not responsive to cortisone and antihistamines as other causes of angioedema.
It is therefore important to make a differential diagnosis in patients with concomitant neoplastic or autoimmune diseases, as its resolution (and thus the patient’s survival) are determined exclusively by administration of the deficient factor C1 inhibitor as well as orotracheal intubation.
References
- Acquired Angioedema. Dtsch Arztebl Int. 2017 Mar 10;114(10):178. doi: 10.3238/arztebl.2017.0178a. Göring HD.
- Drug-induced angioedema: experience of Italian emergency departments. Bertazzoni G, Spina MT, Scarpellini MG, Buccelletti F, De Simone M, Gregori M, Valeriano V, Pugliese FR, Ruggieri MP, Magnanti M, Susi B, Minetola L, Zulli L, D’Ambrogio F. Intern Emerg Med. 2014 Jun;9(4):455-62. doi: 10.1007/s11739-013-1007-x. Epub 2013 Nov 9.
- Urticaria and angioedema. Kanani A, Betschel SD, Warrington R. Allergy Asthma Clin Immunol. 2018 Sep 12;14(Suppl 2):59. doi: 10.1186/s13223-018-0288-z. eCollection 2018. Review
- Idiopathic Nonhistaminergic Acquired Angioedema Versus Hereditary Angioedema. Andrási N, Veszeli N, Kőhalmi KV, Csuka D, Temesszentandrási G, Varga L, Farkas H. J Allergy Clin Immunol Pract. 2018 Jul – Aug;6(4):1205-1208. doi: 10.1016/j.jaip.2018.04.018. Epub 2018 Apr 30
- Hereditary and Acquired Angioedema: Heterogeneity of Pathogenesis and Clinical Phenotypes. Bova M, De Feo G, Parente R, De Pasquale T, Gravante C, Pucci S, Nettis E, Triggiani M. Int Arch Allergy Immunol. 2018;175(3):126-135. doi: 10.1159/000486312. Epub 2018 Jan 26. Review.
- Acquired C1 Inhibitor Deficiency. Otani IM, Banerji A. Immunol Allergy Clin North Am. 2017 Aug;37(3):497-511. doi: 10.1016/j.iac.2017.03.002. Epub 2017 May 15. Review
- Acquired C1-inhibitor deficiency and lymphoproliferative disorders: a tight relationship. Castelli R, Zanichelli A, Cicardi M, Cugno M. Crit Rev Oncol Hematol. 2013 Sep;87(3):323-32. doi: 10.1016/j.critrevonc.2013.02.004. Epub 2013 Mar 13. Review. PMID: 23490322
- Guidance for diagnosis and treatment of acute angioedema in the emergency department: consensus statement by a panel of Italian experts. Cicardi M, Bellis P, Bertazzoni G, Cancian M, Chiesa M, Cremonesi P, Marino P, Montano N, Morselli C, Ottaviani F, Perricone R, Triggiani M, Zanichelli A. Intern Emerg Med. 2014 Feb;9(1):85-92. doi: 10.1007/s11739-013-0993-z. Epub 2013 Sep 4.
- Acquired angioedema in non-Hodgkin’s lymphoma. Healy C, Abuzakouk M, Feighery C, Flint S. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007 May; 103(5):e29-32. Epub 2007 Feb 21. PMID: 1731723
- Treatment with icatibant in the management of drug induced angioedema. Bertazzoni G, Bresciani E, Cipollone L, Fante E, Galandrini R. Eur Rev Med Pharmacol Sci. 2015 Jan;19(1):149-53.

