- Mantuano Stefania
- Brief Report and Case Report
Suspect Moschcowitz syndrome: how, when, why
- 2/2019-giugno
- ISSN 2532-1285
- https://doi.org/10.23832/ITJEM.2019.014
1) Emergency Medicine and Trauma Surgery, Grande Ospedale Metropolitano “Bianchi Melacrino Morelli”, Reggio Calabria
2) Grande Ospedale Metropolitano “Bianchi Melacrino Morelli”, Reggio Calabria

Abstract
An 87-year-old female, who had been suffering of dyspnea and high fever for 4 days, came to our ER in yellow code. She said she had been suffering of dyspnea and orthopnoea for fifteen days even with relatively little efforts.
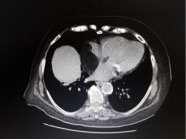
Laboratory data showed the presence of a mass in the right atrial cavity.
The woman was submitted to cardiologic surgery unit to be undergone to a partial neoformation removal operation.
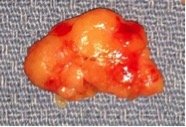
After a histological examination, it was possible to establish that the mass was formed by a benign tumor (Lipoma).
After about thirteen occupant days in our Cardiac surgery unit, the patient moved to a centre of Cardio rehabilitation for the necessary therapies.
Keywords
dyspnea – neoformation – lipoma – cardiac surgery – Cardiopulmonary rehabilitation
Clinical Case
Figure 1
Figure 2
Short historical hints
The primary tumors of the heart in adulthood can be benign or malignant. They have a variable incidence, the frequency of primary cardiac tumors is approximately 0.02%, corresponding to 200 tumors in 1 million autopsies1. The benign tumors are more common than the malignant, at a 3:1 ratio.
Bibliography
- Reynen K. Frequency of primary tumors of the heart. Am J Cardiol 1996; 77: 107.
- Grebenc ML, Rosado de Christenson ML, Burke AP, Green CE, Galvin JR. Primary cardiac and pericardial neoplasms: radiologic-pathologic correlation. Radiographics 2000; 20: 1073-103.
- S Tremosini et al – Sarcoma primitivo del cuore. Descrizione di un caso. G Ital Cardiol 2007; 8 (3): 196-200
- Sarjeant JM, Butany J, Cusimano RJ. Cancer of the heart: epidemiology and management of primary tumors and metastases. Am J Cardiovasc Drugs 2003; 3: 407-21.