- Paolo Pinna Parpaglia
- Original Article
Syncope and head trauma in elderly: a pilot study
- 3/2017-Ottobre
- ISSN 2532-1285
- https://doi.org/10.23832/ITJEM.2017.026
Pinna Parpaglia P. (1), Secci R. (1), Uras C. (2), Oppes M. (2).
1) Syncope Unit, UO Medicina d’Urgenza;
2) UO Pronto Soccorso e Medicina d’Urgenza, AOU Sassari, Italy

Abstract
Falls in elderly represent a major health and social concern, particularly for their traumatic consequences and, among them, for head traumas (HT). The capacity to recognize the cause of fall in elderly is compromised by the difficulty in collecting a reliable description of the event and by the tendency of caring physicians to focus mainly on the consequence of trauma, instead of its mechanism, thus hampering the possibility to implement proper preventive interventions. Syncope in literature is reported as a minor cause of trauma due to fall in elderly, indeed no one study has perspectively and specifically investigated this item in relation to head trauma. We tested in a one month perspective study a brief diagnostic protocol (<24 hours) aimed to define, beside the consequence, the cause of fall in elderly with head trauma, devoting particular attention primarily to the anamnestic capacity and, secondary, to the syncope diagnostic work-up. Unlike the usual ER diagnostic approach for HT, derived from a retrospective analysis of a four-month period in the same ER (control group), the study diagnostic protocol demonstrated that syncope was significantly more frequent than expected (42% vs 14%, p<0,01) in these patients. If these results were confirmed, syncope could be considered the leading cause of HT due to fall in elderly, encouraging ER physicians to implement their HT protocols with a more extensive cause-oriented work-up for this category of patients.
Introduction
Falls represent one of the most challenging problems in the elder population as well as a major health concern, indeed about 35% of people over 65 years old experience at least one fall each year. In this category, falls are responsible of the vast majority of trauma (around 80%) and are the most common cause of traumatic brain injuries (TBI)1,3. TBI in the elderly carries the risk of heavy consequences on mortality and morbidity, as well as on health costs, and is responsible of a huge number, ever increasing, of emergency room (ER) accesses and hospital admissions1. Furthermore, a history of a single fall is a major risk factor for a subsequent new fall, increasing the risk of repetitive TBI2,4. The public health and socio-economic consequences of injuries due to falls in the elderly, and in particular of TBI, impose appropriate preventative intervention policies which could arise only from the full understanding of the causes and mechanisms of falls 5-9,12,14. Indeed, in overcrowded ER, the diagnostic work-up in the traumatic brain injured patient is focused mainly on the consequences, instead of on the causes, of trauma, and the cause of fall is usually attributed by the first physician who takes care of the patient without the appropriate in-depth evaluation. Moreover, elderly frequently do not remember mechanisms of falls and sometimes suffer from amnesia, either pre or post injury, making anamnesis, the most useful tool for explaining the cause of trauma, often useless or very complex and, anyway excessively time consuming for the ever crowded emergency department (ED) 3,11. Since in the elderly it is very challenging the understanding of the cause of fall and indeed exists a significant diagnostic overlap between accidental fall and syncope14, mainly because of the less reliability of the usual medical history collection, UK national STARS program (Syncope Trust And Reflex anoxic Seizures) prepared a questionnaire to submit to patients, to be filled in together with their relatives and possibly with event witnesses, aimed to better clarify the cause of fall10. By the careful interpretation of the answers, physician should be able to exclude or, in turn, to consider certain or highly probable, a syncopal fall. To date accidental falls are considered the leading cause of head trauma in the elderly, accounting for about 70% of them, whereas syncope is estimated to be responsible in only the 2-20% of cases, but such evidences emerge from observational studies and institutional registries, not designed to clarify the cause and mechanism of falls6. Furthermore, it could be expected that head trauma would be more frequent than other kinds of trauma as a consequence of a syncopal flop down without control. This hypothesis would apply in everyday ER practice, unless never proven. Based on the above considerations, it could be argued that syncope could be far more frequent than reported as a cause of head trauma in the elderly. We then underwent a study that used a systematic diagnostic approach aimed to assess the real prevalence of syncope as cause of fall and head trauma in the elderly and compared results with retrospective data from the same ER. The study has been approved by the local ethical committee (prot. 2133/CE, 01/13/2015).
Methods
Study group (perspective group)
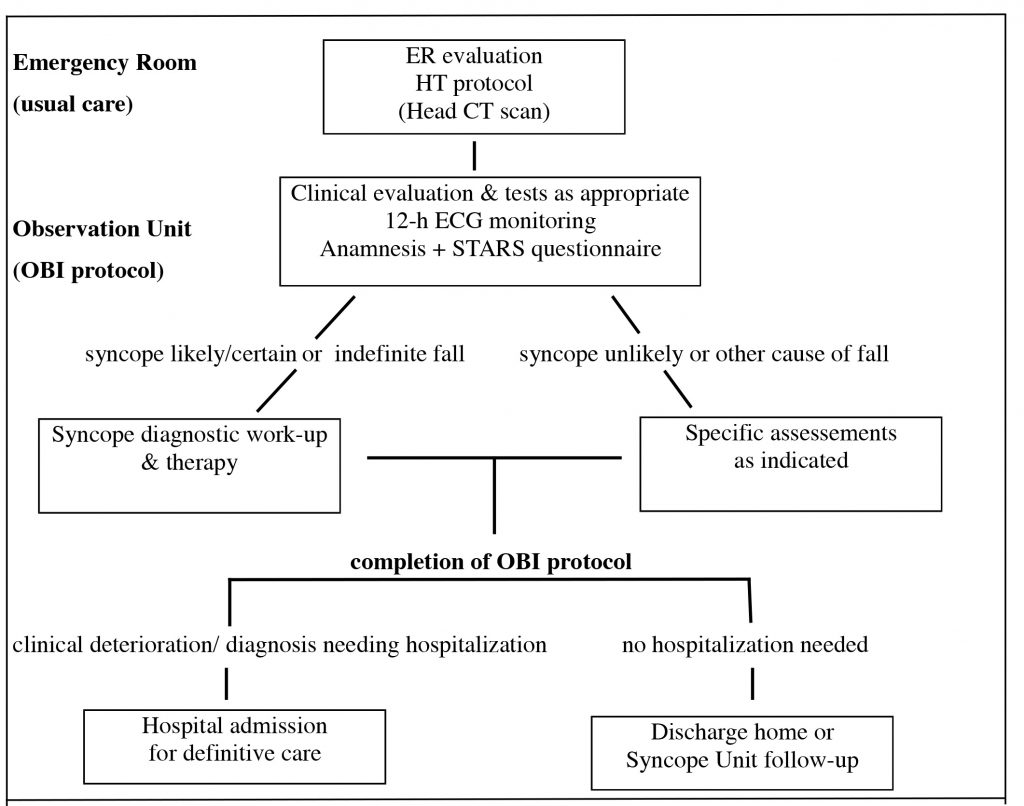
For this purpose, all elder people, aged >65years old, consecutively presented during one month, may 2014, to the ER of the AOU Sassari (Azienda Ospedaliera Universitaria), Italy, complaining head trauma due to fall as the main complain, have been perspectively studied. Study protocol: after the initial ER evaluation, the whole study population underwent a 24 hour diagnostic work-up in the ED Observation Unit (OBI) in order to identify the likely cause of fall, recognizing, at the end of the pathway, one of the four different mechanisms classified below (see Diagnosis). The ER physicians where unaware of the study purpose and where uniquely asked to normally operate and to transfer all patients with the above-mentioned characteristics to the local OBI at the conclusion of normal ER clinical path, which consisted of a general and neurological physical examination, a brief anamnesis, 12-lead ECG, Head CT scan and any other exam the emergency physician believed as appropriate, in accordance with the local head trauma protocol. This ER evaluation represent the usual care for this kind of problem in our institution. The subsequent OBI work-up consisted of a 12 hours continuous telemetry ECG monitoring, clinical monitoring, blood tests as appropriate, a second CT scan if needed and, especially, an in-depth anamnesis, either involving relatives and eyewitnesses, with the completion of the STARS questionnaire expressly translated in Italian. If, after the in-depth anamnesis along with the STARS questionnaire interpretation and the clinical and 12hour ECG monitoring, a certain or highly probable syncopal transient loss of consciousness was considered responsible of the head trauma or if the cause of fall remained undetermined, the patients underwent the syncope diagnostic work-up in accordance with the European Society of Cardiology guidelines13. At the end of the OBI pathway, patients were discharged home or, in case of complication or diagnosis requiring further interventions, transferred to a definitive care. The above diagnostic pathway has been considered as the study “OBI diagnostic protocol” (fig. 1).
Fig. 1: OBI diagnostic protocol flow chart
Control group (retrospective group)
In order to compare the OBI diagnostic protocol to the usual care diagnostic work-up, we retrospectively analysed all the patients with the same characteristics of the study population that consecutively presented to the same ER during a four months period of the year before (March to June 2014). All the patients where treated in accordance with the local standard of care for these kind of problems, as described above. The causes of fall were then extrapolated from the ER medical reports and divided into
the 4 mechanisms (causes) listed below.
In order to compare the OBI diagnostic protocol to the usual care diagnostic work-up, we retrospectively analysed all the patients with the same characteristics of the study population that consecutively presented to the same ER during a four months period of the year before (March to June 2014). All the patients where treated in accordance with the local standard of care for these kind of problems, as described above. The causes of fall were then extrapolated from the ER medical reports and divided into
the 4 mechanisms (causes) listed below.
This diagnostic work-up was considered the “usual care”.
In both groups, in agreement with the study objectives, patients with head trauma secondary to causes different from fall (ie. street accidents, aggressions, etc.) have been excluded.
Diagnosis
Causes of fall have been divided into 4 categories listed below:
1. Syncopal (certain and very likely)
2. Accidental (due to environmental/external causes)
3. Other determinate causes of fall (specified)
4. Indeterminate
Each fall in either group, at the end of the diagnostic work-up, has been attributed to one of the above mentioned four mechanisms.
Statistical Analysis
Continuous data have been expressed as mean (SD). Chi-square tests were used to compare categorical data of syncopal (either certain and very likely) falls vs all other causes of fall (accidental, indeterminate and other) in order to evaluate the difference between groups. P values below 0.05 were considered statistically significant.
Results
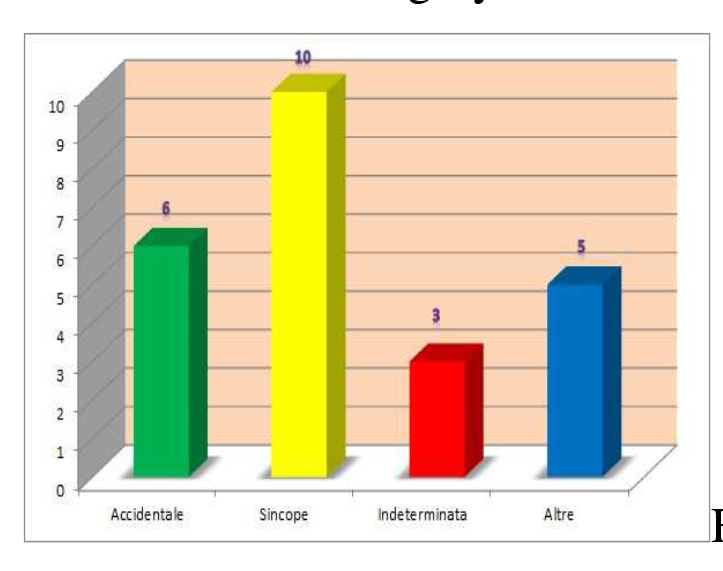
The study group comprised 24 patients over 65 years old, consecutively presented at the ER during one month (may 2015) for head trauma, as mayor injury, due to fall. All the 24 patients (mean age 79+/- 3; males 42%) underwent the OBI diagnostic protocol as described above. At the end of the OBI diagnostic protocol, the detected causes of fall where as follow: 6 accidental, 10 syncopal, 5 other causes and 3 indeterminate. Thus, syncopal causes of head trauma accounted for the 42% of total falls (fig. 2). Among the 10 syncopal falls, 2 were recognized as cardiogenic (high heart rate in paroxismal atrial fibrillation), 5 were due to orthostatic hypotension and 3 were reflex (2 vasodepressives and 1 cardioinhibitory that required pace-maker implantation). The 5 other determinate causes comprised two postural instability, one vertigo, one hyponatremia and one alcohol intoxication. According to the Glasgow Coma Scale (GCS) all head traumas have been classified as mild (GCS 15) but one classified as moderate (GCS 13), whereas the head CT scan revealed six, out of 24, posttraumatic brain injuries (one subarachnoid bleeding, three subdural haematoma one of which required surgical evacuation, one intraparenchimal haemorrhage and one frontal lobe contusion). Three out of six head trauma with brain injuries (50%) where due to syncopal falls and two (33%) where taking warfarin. Seven out of 24 patients have been finally hospitalized (29%): six in the emergency medicine ward and one in the neurosurgery unit.
Fig. 2: causes of fall in the study group (OBI diagnostic protocol).
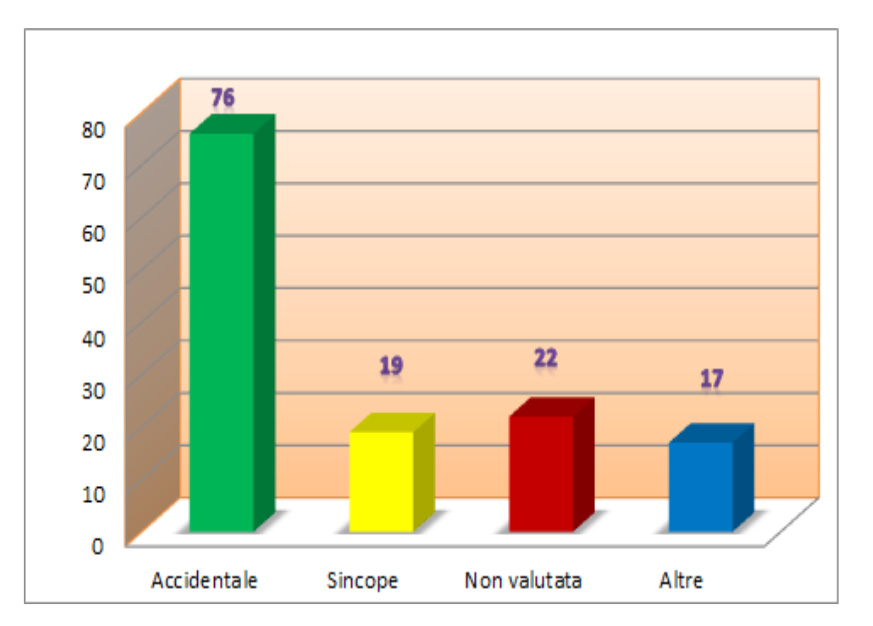
The control group comprised 134 patients, 65 years old or more (mean age 77 +/- 4; males 44%), consecutively presented at the same ER from March to June 2014 for head trauma secondary to fall and treated in accordance with the local head trauma protocol (standard of care). The distribution of the causes of falls extrapolated from ED medical reports was as follow: 76 accidental, 19 syncopal, 17 others, 22 indeterminate. Syncopal episodes accounted for only 14% of total, whereas accidental falls,
accounting for the 57% of causes, were the most frequent (Fig. 3).
No further investigation aimed to find syncope aetiology was reported in this retrospective group.
Fig. 3: causes of fall in control group (usual care).
Comparison between study (OBI diagnostic protocol) and control (usual care) groups
| Causes of fall (diagnosis) | Study Group n=24 (%) | Control Group n=134 (%) |
| Accidental | 6 (25) | 76 (57) |
| Syncopal | 10 (42) | 19 (14) |
| Other | 5 (21) | 17 (13) |
| Indeterminate | 3 (12) | 22 (16) |
| OBI diagnostic protocol (n=24) |
Usual Care (n=134) |
p | |
| SYNCOPAL | 10 | 19 | <0,01 |
| NON SYNCOPAL | 14 | 115 |
<0,01 |
The comparison between the two diagnostic strategies, OBI diagnostic protocol versus usual care, although the number of patients in the study group was fairly scarce, demonstrated a statistically significant superiority of the first strategy in detecting syncope as the plausible cause of falls (10/24 vs 19/134, chi-squared 6,92, p <0,01).
Discussion
The aim of the present study was to validate the insight that syncope could be much more frequent than believed as cause of fall and head trauma in elderly. It’s well established that anamnesis is one of the most powerful diagnostic tool in the evaluation of patients with probable transient loss of consciousness, either to clarify the mechanism of fall and possibly to establish the aetiology of syncope 12. It’s also well known that in elderly patients anamnesis is often unreliable, because of memory deficiency, post-traumatic amnesia and facts misperception, thus rendering the brief anamnesis made in the ever crowded ER probably not effective in determining the true cause of fall. For these reasons an epidemiological overlap exists between syncope and falls in elderly 14. We developed a brief, low cost, observation protocol (< 24 hours) that, beside the usual observation for the consequence of the fall (i.e. head trauma), devoted particular attention to the understanding of the cause (OBI diagnostic protocol). The OBI diagnostic protocol allowed us to diagnose much more transient loss of consciousness and syncopal falls (either certain or highly likely) than did usual care approach. Recognizing syncope as the first cause of head trauma due to fall in elderly. Moreover, it’s been identified the aetiology of syncope in most cases, thus putting the patients in the condition of being treated and possibly of avoiding new syncopal falls. The reported frequency of syncope as cause of fall in elderly is surprisingly low, even lower then in our control population (usual care group), being as low as less than 3% in most studies 13. Although fairly numerous, studies of falls in elderly are very heterogeneous and show significant inconsistencies in research methodologies, including patients selection, study design (mainly retrospectives and observationals) and definitions of fall, thus rendering their interpretation for our purpose (ie. frequency of syncopal falls and head trauma) hardly reliable15. Moreover, none has specifically investigated the frequency of syncope in this category of patients15. On the other end, given the heterogeneity of the definitions of fall and the general difficulties encountered in literature in its classification, we believe that the pre-specified diagnostic simplification, differentiating syncopal from all other non-syncopal cause of fall, strengthen our results. We are aware of the limitations of the present study. Mainly the numerosity of the population studied, indeed very low, but enough to show a large difference between groups. Furthermore, our study has been conducted in a single centre, it is therefore possible that in other institutions the usual care for these patients could be much more oriented toward recognition of syncopal falls, although, as far as we know, the concerning data are not reported in literature. Moreover, the diagnosis of syncope wasn’t made by definite tests but it derived basically from medical judgement and provocative tests, thus prone to to some extent of subjectivity, although achieved at the end of a comprehensive observational protocol. Anyway, it should be considered that a reliable anamnesis is still the most powerful tool available for differentiating transient loss of consciousness from other causes of fall 10, whereat we believe that our protocol allowed us to approach as closer as possible to the true cause of fall, even though we are fairly conscious that a diagnostic certainty in this topic is not possible so far. Another explanation possibly responsible, at least in part, of the results, is the fact that syncope can cause head trauma more frequently than other causes of fall, because the uncontrolled fall, as syncopal one is, could have per se a higher probability to hit the head16. The enlargement of the study population will probably give answer also to this topic. Finally, unless the study sample is too small to establish the real incidence of the different aetiologies of syncope, it is noteworthy that the recognition of the syncopal falls, in most cases enabled us to carry out a focused therapy in order to prevent new episodes, even if we must be aware of other mechanisms of fall that will possibly cause new traumas.
Conclusions
Our study demonstrated that a brief diagnostic protocol aimed to establish the cause of fall in head trauma elderly patients can help to diagnose much more syncopal falls than otherwise observed when the diagnostic pathway is predominantly oriented toward trauma consequences. If these results would be confirmed in a larger study, ER protocols for trauma due to fall in elderly should consider a more comprehensive syncope diagnostic work-up.
References
- Thompson HJ et al. Traumatic Brain Injury in Older Adults: Epidemiology, Outcomes, and Future Implications. J Am Geriatr Soc . 2006 October ; 54(10): 1590–1595.
- Tinetti ME. Clinical practice. Preventing falls in elderly persons. N Engl J Med 2003;348:42–49.
- Langlois, JA et al. Traumatic Brain Injury in the United States: Emergency Department Visits, Hospitalizations, and Deaths. National Center for Injury Prevention and Control; Atlanta, GA: 2004.
- US Bureau of the Census. US Administration on Aging. Older Population by Age, 1900–2050 [August 11,2005]. www.aoa.gov/prof/Statistics/online_stat_data/AgePop2050.asp
- Magaziner J et al. Predictors of functional recovery one year following hospital discharge for hip fracture: a prospective study. J Gerontol Med Sci 1990;45:M101– 7.
- Sattin RW et al. The incidence of fall-injury events among the elderly in a defined population. Am J Epidemiol 1990;131: 1028– 37.
- McKevitt EC et al. Geriatric trauma: Resource use and patient outcomes. Can J Surg 2003;46:211–215.
- Traumatic Brain Injury in the United States. A Report to Congress. Centers for Disease Control and Prevention; Atlanta, GA: 2001.
- Hukkelhoven CW et al. Patient age and outcome following severe traumatic brain injury: An analysis of 5,600 patients. J Neurosurg 2003;99:666–673.
- www.stars.org.uk
- Kenny RA et al. “Transient loss of consciousness, syncope and falls in the elderly”. Blackwell Publishing Company, Inc. Armonk, New York, 2001.
- High Diagnostic Yield and Accuracy of History, Physical Examination, and ECG in Patients with Transient Loss of Consciousness in FAST: The Fainting Assessment Study Van Dijk N et al. J Cardiovasc Electrophysiol, 2008; 19:48-5
- Guidelines for the diagnosis and management of syncope. European Heart Journal (2009) 30, 2631–2671
- F. E. Shaw, R. A. Kenny. The overlap between syncope and falls in the elderly. Postgrad Med J 1997;73:635-639.
- Masud T, Morris RO. Epidemiology of falls. Age and Ageing 2001; 30-S4: 3–7.
- Nevitt MC et al. Risk factors for injurious falls: a prospective study. J Gerontol 1991;46:M164–70.