- Giacomo Veronese
- Brief Report and Case Report
What makes emergency medicine residents satisfied? A web based national survey
- 2/2017-Giugno
- ISSN 2532-1285
- https://doi.org/10.23832/ITJEM.2017.015
 Giacomo Veronese, MD1; Alberto Broggi, MD2; Eleonora Serra, MD3; Efrem Colonetti, MD2, Stefano Geniere Nigra, MD4
Giacomo Veronese, MD1; Alberto Broggi, MD2; Eleonora Serra, MD3; Efrem Colonetti, MD2, Stefano Geniere Nigra, MD4- Department of Emergency Medicine, Ospedale Niguarda Ca’ Granda, University of Milano- Bicocca, Milan, Italy
- Department of Emergency Medicine, ASST degli Spedali Civili di Brescia, University of Brescia, Brescia, Italy
- Department of Emergency Medicine, Azienda Ospedaliero-Universitaria di Parma, University of Parma, Parma, Italy
- Department of Emergency Medicine, Policlinico San Matteo Pavia Fondazione IRCCS, University of Pavia, Pavia, Italy
Abstract
In Italy, a five-year emergency medicine residency training program was born in 2008. From November 2015 to January 2016 a cross-sectional national survey was launched to all residents enrolled in every Italian emergency medicine residency program. The purpose was to collect descriptive data on how each residency program was organized. Furthermore, the satisfaction rate of medical trainees was inquired. Residency is a key period for every doctor and we thus believe that attention towards potential target factors that might be implemented to build a successful training program is mandatory.
Brief Report
In Italy, a five-year emergency medicine residency training program was born in 2008. Italian residency program guidelines issued by the Ministry of Education, Universities and Research define the goals to be achieved at the end of the 5-year training but do not clearly specify how these have to be reached [1]. Every single university thus set up its own residency program (i.e. in terms of clinical rotations, lectures, etc.) leading to possible heterogeneity in national training. A team of residents enrolled in this relatively young training program gathered together in 2010 forming a national association called Coordinamento degli Specializzandi in Medicina d’Emergenza-Urgenza (CoSMEU) with the aim of monitoring and improving the emergency medicine training in Italy [2]. Valuable sources for evaluating a successful residency are the opinions of the residents themselves. Thus, in 2015 CoSMEU launched a cross-sectional national survey to all the residents enrolled in every Italian emergency medicine residency program. The purpose was to collect descriptive data on how each residency program was organized among the five-year training and which kind of knowledge and skills were acquired during the education period. Furthermore, the satisfaction rate of medical trainees was inquired and factors that correlate residents’ satisfaction with their residency experience and education were investigated. From November 2015 to January 2016, 2nd- to-5th year resident physicians enrolled in Italian emergency medicine training programs were recruited to this study by distributing the survey via institutional email. Informed consent was attained for all research participants. Medical residents then completed the electronic (computer- based) survey and responses to survey questions were collected anonymously, were de-identified, and were stored under password-protection online. Participants had the option of terminating the survey at any point. Surrogates of satisfaction corresponded to a score ≥ 6 in a scale between one (totally unsatisfied) to ten (totally satisfied) and/or to a negative answer to the question “Have you ever thought about changing your residency training program?”. Using logistic regression, the analyzed potential predictors of residents’ satisfaction were: first, feeling oneself confident among eight emergency medicine-related areas, including medical emergencies, surgical emergencies, pediatric emergencies, obstetric and gynecological emergencies, cardiac arrest management, trauma management, emergency ultrasonography, and non-invasive ventilation management; second, feeling oneself autonomous among specific emergency physician technical skills, i.e. establishing a central venous access, placing a chest tube, orotracheal intubation and mechanical ventilation management, procedural sedation and analgesia, loco regional anesthesia, electrical cardioversion procedure, and fracture / dislocation reduction. Besides we investigated the quality of the lessons, the opportunity to join research projects related to emergency medicine, the involvement in teaching
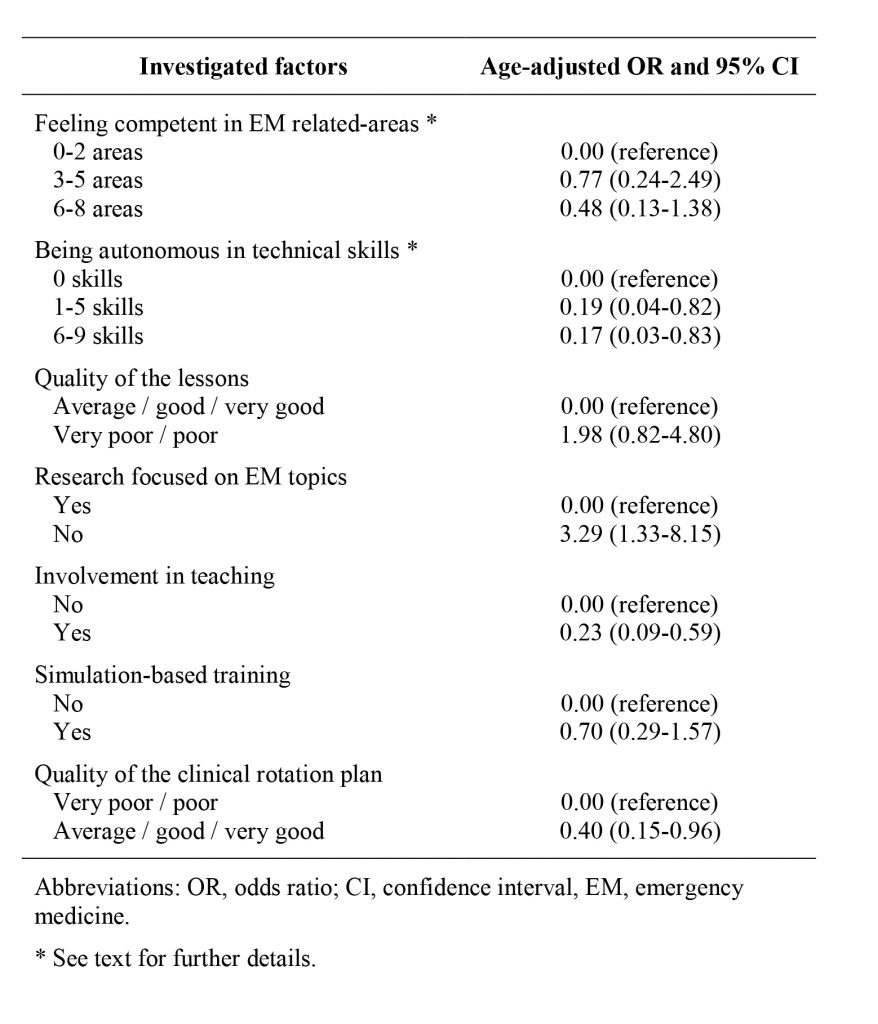
to younger colleagues or students, the presence of simulation-based learning and the quality of the clinical rotation plan. All analyses were carried out using STATA (version 12 SE, Stata Corp, College Station, Texas, USA). This study adhered to the tenets of the 1964 Helsinki declaration and its later amendments or comparable ethical standards. A total of 89 emergency medicine residents from 20 different national universities participated to the survey, that was 30.5% of the total Italian 2nd-to-5th year emergency medicine trainees in January 2016. Clinical rotation plan and length are summarized in Figure 1. Among the participants, there were 55 residents (61.8%) satisfied with the residency program they were attending. Factors related to residents’ dissatisfaction are detailed in Table 1. It was found out that a protective factor against dissatisfaction was estimating oneself competent in more than three areas out of the eight inquired by the survey (age adjusted odds ratio [aOR] 0.77, 95% confidence interval [95%CI] 0.24-2.49 for 3-5 areas and aOR 0.48, 95%CI 0.13- 1.38 for 6-8 areas) with respect to those who declared to be confident in less than three fields. Being also autonomous in specific technical skills, with or without a supervision, gave similar results: the aOR was 0.19 (95%CI 0.04-0.82) if 1 to 5 skills were involved, and 0.17 (95%CI 0.03-0.83) if 6 or more skills were involved compared to feeling not autonomous in any of the investigated abilities. Poor quality lessons were related to dissatisfaction (aOR 1.98, 95%CI 0.82-4.80), as well as the lack of research project proposals focused on emergency medicine (aOR 3.29, 95%CI 1.33-8.15). On the contrary, the presence of simulation-based learning for trainees (aOR 0.70, 95%CI 0.29-1.57), being involved in teaching to younger colleagues or medical students (aOR 0.23, 95%CI 0.09-0.59), and good perceived five-year clinical rotation plan (aOR 0.40, 95%CI 0.15-0.96), were all items related to residents’ satisfaction. The results of the study, even though partially comparable and setting- specific, are in line with existing evidence focused on other residency programs [3-5]. This survey showed a picture of a newborn residency program, highlighting the needs of its physicians in training. Residency is a key period for every doctor and we thus believe that attention towards potential target factors that might be implemented to build a successful training program is mandatory. Considering the recent birth of the emergency medicine residency program, further assessments are important to examine how this is evolving through the years.
Acknowledgments
The authors thank all members of Coordinamento degli Specializzandi in Medicina d’Emergenza- Urgenza (CoSMEU) and all residents who took part into the study. This study did not receive any grants or funding. All authors had no competing interests to declare. The work has been presented orally during the X Italian Congress of Emergency Medicine (Naples, 18/20 November 2016). All authors have seen and approved the manuscript and have contributed significantly to the work.
Table 1: Factors associated with the risk of dissatisfaction among a cohort of Italian residents in emergency medicine.
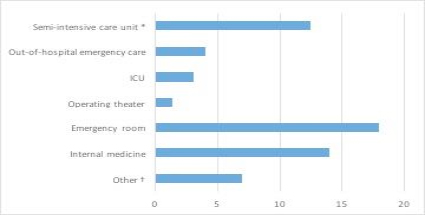
Figure 1: Clinical rotation plan and length (horizontal axis, mean duration in months) of the emergency medicine residency training program (national perspective from 20 universities). Abbreviations: ICU, intensive care unit.
- Wards provided with multi-parameter monitors, ultrasound devices, vasopressor support, noninvasive mechanical ventilation.
- Includes Cardiology, Acute Coronary and Respiratory Care Unit, Pulmonology, Radiology, Geriatrics, Endocrinology, Stroke Unit, Infectious Diseases, Obstetrics & Gynecology, Eye Ear and Throat unit, Orthopedics.
References
- Ministero dell’Istruzione, dell’Università e della Ricerca. Available at: http://attiministeriali.miur.it/UserFiles/2292.pdf
- Coordinamento Specializzandi in Medicina d’Emergenza-Urgenza (CoSMEU). Available at: https://cosmeu.wordpress.com
- Lam CZ, Nguyen HN, Ferguson EC; Radiology Resident’ Satisfaction With Their Training and Education in the United States: Effect of Program Directors, Teaching Faculty, and Other Factors on Program Success. AJR Am J Roentgenol 2016; 206(5):907-916.
- Guffey D, Feldman SR, Huang WW; What are the most important factors that determine the overall quality of dermatology residency training: A resident survey. Dermatol Online J 2015; 21(10). pii: 13030/qt0j11p97g.
- Smallwood N, Krishnamoorthy S; Acute Internal Medicine Trainee Survey 2016. Acute Med. 2016;15(2):93-97.