- Paola Noto
- Original Article
Diagnostic accuracy of integrated clinic ultrasound in critically ill
- 3/2016-Ottobre
- ISSN 2532-1285
Elisa Basile ° , Paola Noto*,Luca Ruggeri* , Giuseppe Carpinteri*
° MCAU Azienda Ospedaliera Santa Croce e Carle- Cuneo
*MCAU Azienda Ospedaliero-Universitaria Policlinico Vittorio Emanuele – Catania
Abstract
Background
Our study was aimed at demonstrating how the integrated use of clinic ultrasound, in addition to the “standard” medical assessment optimizes diagnostic accuracy in the differential diagnosis of dyspnoeas, shocks and bronchopneumonic consolidation.
Materials and methods
We enrolled 106 patients, of average age 75 years (SD +/- 12), 50% males and 50% females. The admission diagnosis was formulated in a “standard” way, i.e. through EO, medical history, ECG, EGA, laboratory and radiological examinations (chest and / or abdomen X-ray and / or chest and / or abdomen CT). Within 12 hours from the access to the ward, an integrated ultrasound examination of thorax-heart-VCI-abdomen-vessels was performed, starting from the chest in patients with B-failure, or from the VCI in C-failure ones, in order to formulate an intermediate ultrasound diagnosis . At discharge, a final diagnosis was given, considering the level II of investigations, the clinical course and the response to therapy.
Results
Compared to the final diagnosis, the integrated ultrasound had changed the admission diagnosis in 35% of patients, confirming this in 60% of cases ; 5 ultrasonographic diagnoses were rather incorrect than the final ones (4%). The ultrasound examination has increased the diagnostic accuracy especially in the diagnosis of acute cardiogenic pulmonary edema (APE) and of the mixed dyspnoea .The US has demonstrated greater accuracy in the diagnosis of FBP (Pulmonary Fibrosis) than standard radiographic examination. The clinical evaluation has rather had high sensitivity (84%) in the diagnosis of hypovolemic/ distributive shock , producing an overestimate of cardiogenic shock cases, and an underestimation of the mixed forms. Finally, it has highlighted positive correlation between commitment AI score> 12 and mortality, and with the need for higher FIO2> 50% and / or application of a PEEP.
Conclusions
In the light of the results obtained, we believe that the proposed integrated ultrasound protocol can be a tool that can significantly improve the diagnostic accuracy approach in the short of breath patient and / or in shock
Introduction
Over the past two decades we have seen a flowering of literature about the usefulness of clinic ultrasonography in Emergency, when applied in the territory, in the Emergency Departments and in the field of intensive care, but little evidence comes from sub-acute care areas and non-intensive ones as departments of Internal Medicine and Urgency. From the reported evidence in literature, consequent indications and algorithms are built on the use of ultrasound in critical frameworks, such as the arrest, the periarrest and those conditions with a high risk of evolution, where the assessment must be quick and with high diagnostic and therapeutic impact in order to influence positively the prognosis (1,2). The ultrasound applied in the emergency wards responds to simple questions that come out during the initial assessment of the sick, using an approach described by some authors as “visual medicines” (3). It should however be noted that the correct interpretation of the acquired ultrasound data is closely linked to the ABCDE assessment, medical history and physical examination, as well as the replies from the biochemical and instrumental investigations performed at the bedside (ECG, EGA, Chest X-ray) .
These considerations led to the idea of assessing to what extent, including in relation to non-intensive care, the use of an integrated ultrasound Protocol (chest, heart, blood vessels and abdomen) may improve diagnostic accuracy, in terms of increased sensitivity and specificity, the critical management of the sick suffering from B-failure and / or C-failure, compared to a “standard” approach such as clinical – medical- radiological tests.
Materials and methods
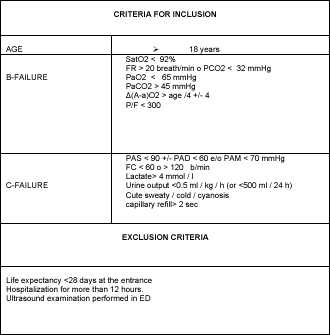
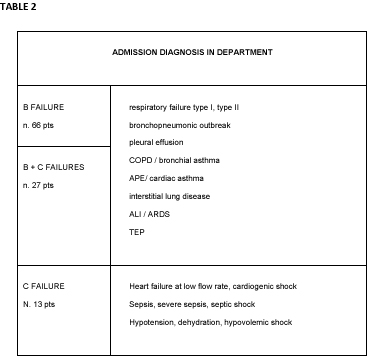
Table 1 shows criteria for inclusion and exclusion. None of the patients enrolled had performed ultrasound investigation in ED, so the diagnosis of admission to the ward (Table 2) was formulated in a “standard” way by the emergency room physician, or mail based on physical examination, medical history, laboratory tests, ECG, chest X-ray and EG
For each eligible patient admitted to the ward, within 12 hours from the access, a medical history has been collected and a physical examination has been performed, integrating with ECG data, blood gas, radiographic (chest and / or abdomen X -ray, chest and / or abdomen CT) and laboratory tests (blood count, CRP, NTproBNP), confirming the diagnosis of admission that was formulated in the emergency room.
When prompted by the case, there were collected biological samples for culturing, or run the HS troponin assays, D-Dimer, procalcitonin.
The clinical and medical history evaluation was then implemented by the integrated ultrasound examination, performed by the same doctor who had taken charge of the patient and therefore knew the diagnosis of admission; on the basis of clinical epidemiology data, the ultrasound examination started from the chest in the short of breath patient, or from the VCI in the patient in shock. For the study of the chest there were performed rapid longitudinal and transverse scans along the mid-clavicular lines, anterior and posterior axillary, ideally dividing each hemithorax in 6 fields, upper and lower, medial and posterior; to each field explored it is assigned a score of interstitial commitment, from 0 to 3, so that the total score is hypothetically variable from 0 to 36.
For the study of the heart scans were performed under costal 4-5 rooms and possibly apical and parasternal, according to short and long axes, if the information obtained were not satisfactory. It has been taken over the possible dilation of the cardiac chambers, ventricular hypertrophy and movement of the walls (hypo / akinesia, dyskinesia and hyperkinesia); It was also estimated the systolic function of the left and right ventricle (respectively using the inspection method or the fractional shortening and the estimated TAPSE), as well as diastolic function of the left ventricle using the E / A ratio. Finally it made an inspection assessment of flap valves and atrioventricular with estimates of PAPS, and it has been researched the possible pericardial effusion.
For the study of the deep veins we used transverse scans of the groin and the popliteal fossa with the compression ultrasonography (CUS), in order to search for partial or complete signs of deep vein thrombosis.
Abdominal ultrasound was done in accordance with transverse scans, longitudinal and oblique ones, looking for free fluid in the most dependent sectors, vascular abnormalities, alterations of the hepatic parenchyma and biliary tract, abnormal urogenital district and intra-abdominal and pelvic masses .
Each pathologic finding was recorded on a database (5) leaving paraphysiological sonographic findings or mild disease of no clinical relevance (calcification, vascular atheroma not significant, renal cysts, kidney stones and gallbladder without expansion or signs of inflammation ).
Based on ultrasonographic findings, interpreted in the light of the clinical and laboratory data, it was formulated for each patient an intermediate ultrasound diagnosis.
At the time of discharge, a final diagnosis was placed by the responsible of the medical staff. It took into consideration any II level investigation performed during hospitalization, the clinical course and the response to medical therapy: the discharge diagnosis was considered the gold standard for subsequent statistical analysis.
Therefore we performed measurements of descriptive statistics and calculated the agreement of the two methods (standard and ultrasound ones) to identify the discharge diagnosis. We then calculated the sensitivity and specificity of the clinical method and the integrated ultrasound method compared to the final discharge diagnosis, in particular for the diagnosis of cardiogenic dyspnea, respiratory and mixed dyspnea, bronchopneumonic consolidation, cardiogenic, hypovolemic/distributive and mixed shock . Finally, we applied the analysis of the ROC curve to the scores of alveolar-interstitial commitment in order to identify the best cut-off, and to correlate this limit to the hospital mortality by performing a comparison of percentages.
Table 1
Results
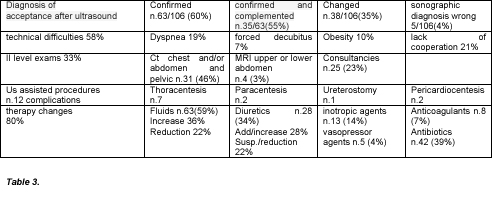
In 60% of the cases the diagnosis of acceptance and the ultrasound match the discharge diagnosis (n. 63 confirmed diagnoses out of 106 cases). In 35% of the cases the diagnosis of acceptance did not equaled the final diagnosis, while the ultrasound was concordant with it (n. 38 changed diagnosis out of 106). In 4% of the cases the ultrasound diagnosis was not coincident to the final diagnosis (n. 5 missed / wrong diagnostic ultrasound in 106 patients). In no event the discharge diagnosis shall not equaled the diagnosis of acceptance, or the ultrasound. In 35 out of 63 patients whose diagnosis was confirmed (55%), ultrasound has added significant clinical elements.
Table 3 shows the descriptive statistical data derived from the study.
We therefore evaluated the diagnostic accuracy of clinical-laboratory and radiological method and the integrated ultrasound method in comparison to the final discharge diagnosis, in the differential diagnosis between cardiogenic, respiratory and mixed dyspnea.
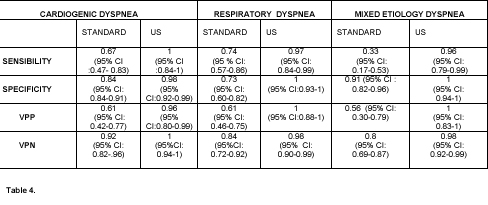
In the diagnosis of cardiogenic APE (31/106), the sensitivity and specificity was respectively 0.67 and 0.84 for the standard method, and 1 and 0.98 for the integrated thoracic and cardiac ultrasound. In the diagnosis of respiratory dyspnea, including the diagnosis of COPD exacerbation (10/106) bronchopneumonic consolidation (29/106), interstitial lung disease (8/106), TEP (7/106), ALI / ARDS (7/106), massive pleural effusion (2/106) and post-traumatic pulmonary contusion (2/106), the standard method has shown to have sensitivity of 0.74 and specificity of 0.73; for the integrated ultrasound examination instead, the diagnostic accuracy was respectively 0.97 and 1.
In Table 4 are reported the results obtained with the associated confidence intervals of 95%.
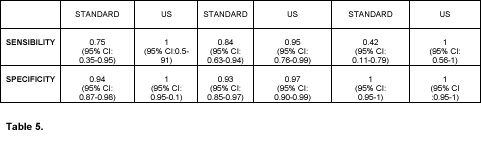
Regarding to the diagnosis of bronchopneumonic consolidation, the standard method had sensitivity and specificity of respectively 0.7 and 0.81. The use of thoracic ultrasound has high diagnostic accuracy, with sensitivity of 0.96 and specificity of 0.92.
As for the differential diagnosis of states of shock, the standard evaluation has had sensitivity and specificity of respectively 0.75 and 0. 94 in detecting the cardiogenic shock (8/106 cases), while the integrated ultrasound method had accuracy of 100%. In hypovolemic/distributive shock diagnosis (25/106 cases), the standard method had sensitivity of 0.84 and specificity of 0.93; the ultrasound method instead had values of respectively 0.95 and 0.97. Finally, in detecting the shock with mixed etiology (7 cases out of the total), the standard method has had a low sensitivity of 0.42, while the integrated ultrasound has had 100% accuracy.
It was found a positive correlation between mortality and high score of interstitial-alveolar commitment to chest echo. As a definite cut-off has not already being known in literature, we applied the analysis of the ROC curve (Receiver Operating Characteristic) to the scores used in the sample: on the basis of values of Positive Likelihood Ratio and Negative Likelihood Ratio, we have obtained that the limit value of 12 is probably the best cut-off able to predict mortality.
After the best cut-off was determined, we have divided all patients into two groups according to the score, the first group consists of 63 patients with scores from 0-11, the second consisting of 21 patients with score> = 12. There were found 10 deaths in the first group and 12 deaths in the second group. The comparison of percentages showed a statistically significant difference between the two groups (p = 0.016).
Discussion
Analyzing the results, it is clear that integrating standard assessment of the critically ill patient with an extended multidistrict ultrasound examination, it can be increased the diagnostic accuracy of medical evaluation itself, improving the sensitivity and specificity of the diagnosis.
In particular, the ultrasound examination has permitted to change the diagnosis in one -third of patients (35%), orienting to a more correct therapy sometimes in a decisive way. The data obtained were slightly higher than those described in a study conducted in intensive care (4) where ultrasound is correlated with a higher percentage of non-diagnostic or poor examinations (13% ), an event to be related to the increased complexity of the studied population .
In our study, in over half of the cases in which the admission diagnosis was confirmed (60%), useful elements to a more correct management of the patient have been added, for example, there has been a clamped aortic stenosis or a hypertensive heart disease in patients with APE. These findings have led us to prefer the use of CPAP rather than diuretics; or else there was evidence of a FBP as a cause of COPD exacerbation or undefined sepsis, or cardiomyopathy related to sepsis, which require more careful management of fluid therapy and a more cautious use of amine.
The integrated ultrasound missed the diagnosis in 5 cases out of the total (4%): in particular it was a case of sepsis in supposed pyelonephritis, not confirmed with contrast-enhanced CT; a case of sepsis in cholecystectomy with lithiasis of the intrahepatic bile ducts, not shown in echo because of intestinal bloating; a case of respiratory failure in hilar pneumonia, not viewable in chest echo, and finally two cases of submassive TEP detected with CT angiography.
In the approach to the short of breath patient, the ultrasound examination improves accuracy compared to the single laboratory-clinical-radiological assessment, in particular in APE cardiogenic diagnosis and mixed dyspnoea; in the latter group the sensitivity was very low (0:33), data which indicates how easily one or more causes of dyspnea remain undiagnosed, but the addition of the cardio-thoracic ultrasound assessment has increased the sensitivity over 40%. Furthermore, the standard method tends to overestimate the cases of respiratory dyspnea (47 diagnoses against 39 cases at discharge), while initial diagnosis of cardiogenic dyspnea (n. 30) are numerically superimposable to the number of final diagnoses (n. 27), but with poor correlation of the data because of the many positives and negatives false. This could indicate that the clinic assessment is sufficiently able to identify the respiratory dyspnoea, and often fails to identify the cardiogenic component of dyspnea.
This data also shows in an interesting single-center study conducted by Ray et al. in an emergency department (5)
In our study, in the identification of cardiogenic APE, the integrated thoracic and cardiac ultrasound showed high sensitivity. This is in line with those reported in literature: a study by Cibinel et al. (6) in an emergency department, reported sensitivity and specificity values of thoracic ultrasound respectively of 94% and 84%, much higher than the chest X-ray (66% and 77%). That is to say that the negative predictive value of chest ultrasound is very high (91%) in the exclusion of the cardiogenic APE, while the positive predictive value is slightly lower (87%), because of lower specificity of ultrasound findings of interstitial syndrome. It should be pointed out that the finding of interstitial syndrome ultrasound, compared with a high sensitivity in allowing a first basic distinction between “wet lung” and “dry lung,” has a lower specificity.
As for the diagnosis of bronchopneumonic consolidation, in our records the chest ultrasonography has shown to have greater sensitivity and specificity than standard chest radiography (96% and 92% comparing to 72% and 83%). This is in line with similar studies that compare the accuracy of thoracic ultrasound with traditional radiography for the most common causes of respiratory failure (7). The increased sensitivity is due probably to the ability of ultrasound to better distinguish pleural effusion from consolidations, both radiopaque radiographic examination, and the ability to view the air bronchograms, highly specific for inflammatory consolidations (8). The chest X-ray examination in fact, that has primary indication in the study of pleural-parenchymal diseases, has low sensitivity to small pleural effusions, no more than 45% according to one study (9), partly due to the underestimation of the supine position of the patient during the exam and the need to have at least 200 ml of fluid in the pleural cavity. As for the data relating to the cases of C-failure, in our study the clinical evaluation identified correctly 21 out of 25 cases of hypovolemic / distributive shock (84%), demonstrating sufficient reliability of clinical diagnosis without the aid of ultrasound. This is confirmed in literature: an Italian study has found a high correlation between clinical assessment and ultrasound in the evaluation nontraumatic hypotension (Cohen’s k = 0.710, 95% CI 0614-0806) (10).
The standard method has more difficulty in cardiogenic shock diagnosis (sensitivity 0.74), which was often overestimated (11 cases compared to 8 final diagnosis), and especially in the clinical diagnosis of mixed component shocks (sensitivity 0.42), often underdiagnosed (3 out of 7 final diagnosis cases). It’s basically the cases whose management is more complex, since they are such hypovolemic and heart disease patients, or sepsis complicated by TEP or those who develop hypokinetic heart disease related to sepsis (11): these are the cases, in our opinion, in which the use of VCI-heart-thorax-veins integrated ultrasound can really change the diagnosis and thus direct to the best treatment, avoiding medication errors which put at risk a patient already unstable.
Moreover, it is known as in recent times the validity of only EGDT ( Early Gold Directed Therapy) in the management of patients in septic shock has been widely questioned, with particular reference to the excessive importance given to the PAM values, central venous pressure (PVC) and central venous saturation O2 (ScvO2) (12). Always, one of the most relevant problems in septic patient management was to find the variables that are predictors of the fluids response; in fact, if by one hand the early and aggressive administration of liquids is able to counteract the hypotension, tissue hypoperfusion and organ damage, it is shown that an incongruous fluid administration in septic patients is associated
Therefore, we believe, in view of the above, it is necessary to integrate the clinical and respiratory gas assessments, with visual and functional data, quickly obtainable with an integrated ultrasound examination, useful both in the diagnostic phase and in the subsequent management of the patient in shock. Hemodynamic monitoring through ultrasound study of the respiratory excursions of the VCI (Table 9), which correlates well with an estimate of PVC and fluid responsiveness (14), together with the search of the early appearance of chest B lines in volume expansion and the evaluation of the left contractile function can induce decisive therapeutic choices, for example a more early use of inotropes, that according to the protocol of Rivers, should be reserved for patients with SvcO2 <70% despite transfusion of packed cells (11).
Finally, we consider important the correlation found between the score of interstitial-alveolar commitment in pulmonary edema and mortality. From the analysis of the performed ROC curve, it is clear that by increasing the interstitial commitment score, mortality increases, with specificities that reaches 88% for a score of 12 (p> 0.01), and even 100% for values > 20. We therefore believe that the cut-off of 12 is a valid predictor of mortality index in critically ill patients, as specific sign of extended impairment of alveolar-capillary bed, especially in septic patients, where the pulmonary involvement is often recognized too late and determines poor prognosis.
Interestingly, the patients who died had at least two or more pathological ultrasonographic findings (eg bronchopneumonic consolidation in CMD, or severe sepsis / septic shock, respiratory failure), and it was mostly septic patients suffering from cardiac and onco-hematological basic diseases. In addition, patients with a higher score have necessitated high flow oxygenation systems and / or positive pressure with high FIO2, often> 50%, indicating severe impairment of gas exchange and intrapulmonary shunt. This figure is confirmed by an interesting Spanish study that found an inverse correlation between interstitial engagement score and relationship Fio2 / PO2 (15).
Conclusions
In the light of the results obtained, we believe that the proposed integrated ultrasound protocol can be a tool that can significantly improve the diagnostic accuracy approach in the short of breath patient and / or in shock. This is especially true for the diagnosis of cardiogenic dyspnea, bronchopneumonic consolidation and respiratory disorders, and / or mixed cycle, which recognize several concomitant causes. The diagnosis of hypovolemic/distributive shock was not much affected by the addition of ultrasound examination in terms of significant increase in sensitivity and specificity, however, it made it possible to rule out cardiac involvement as a primary disorder or associated with other causes in determining the state of shock .This protocol has shown to be able to modify the diagnosis and subsequent clinical course in a third of the patients (35%), percentage of cases that we consider significant. Finally it has allowed us to obtain a interstitial commitment cut-off equal to 12, usable as a predictor of mortality. However, additional studies involving a greater number of patients are needed in order to further validate the obtained results.
Bibliography
1) ACEP -American College of Emergency Physicians. Emergency ultrasound guidelines. Ann Emerg Med. 2009.
2) ACEP -American College of Emergency Physicians. Emergency ultrasound imaging criteria compendium. American College of Emergency Physicians. Ann Emerg Med. 2006.
3) Cibinel GA, Martini A. Questo paziente è in arresto cardio-respiratorio? Per quale causa? Decidere in Medicina. 2005;
4) Manno EP, Navarra M, Bertolaccini L, Evangelista A, et al. Deep impact of ultrasound in the Intensive Care Unit: The “ICU sound protocol”. Anestesiology 2012.
5) Ray P, Birolleau S, Lefort Y, Becquemin MH, Beigelman C, Isnard R et al. Acute respiratory failure in the elderly: etiology, emergency diagnosis and prognosis. Crit Care. 2006.
6) Cibinel GA et al. Diagnostic accuracy and riproducubility of pleural and lung ultrasound in discriminating cardiogenic causes of acute dyspnea in the Emergency department. Intern Emergency Medicine 2012.
7) Cortellaro F, et al. Lung ultrasound is an accurate diagnostic tool for the diagnosis of pneumonia in the emergency department. Emerg Med J 2012.
8) Soldati G. Sonographic findings in pulmonary diseases. Radiology Med 2006.
9) Grimberg A, et al. Diagnostic accuracy of sonography for pleural effusion: a systematic review. SanPaolomed J 2010.
10) Volpicelli G, Cardinale L, Stefanone V, Francisco MF et al. Point-of-care multiorgan ultrasonography for the evaluation of undifferentiated hypotension in the emergency department. Intensive Care Med. 2013.
11) Romero-Bermejo FJ , Huertos-Ranchal MJ , et al. Sepsis-induced Cardiomyopathy. Curr Cardiol Rev 2011.
12) Barochia AV, PQ Eichacer, et al. Bundled care for septic shock: an analisys of clinical trials. Crit Care Med 2010.
13) Boyd J, Russel J: Fluid resuscitation in septic shock: a positive fluid balance and elevated central venous pressure are associated with increased mortality. Crit Care Med 2011.
14) Muller L, Molinari N, et al. Respiratory variation of inferior vena cava diameter to predict fluid responsiveness in spontaneously breathing patient with acute circulatory failure: need for a cautious use. Crit Care 2012.
15) Thiago MS, Franci D, Ribeiro D,Carvalho Filho MA et al. A simplified ultrasound-based edema core to assess lung injury and clinical severity in septic patiens. Amer J Emer Med 2013.