- Alberto Giuseppe Guido Piacentini
- Review
A successful prolonged resuscitation in normotermic patient not eligible to extra-corporeal life support
- 1/2018-Febbraio
- ISSN 2532-1285
- https://doi.org/10.23832/ITJEM.2018.003
Alberto Giuseppe Guido Piacentini1 , Andrea Borromini2, Nicolas Martinelli2, Francesco Maggiore2, Davide Cattano3, Geza Halasz4
Abstract
Background: Out of hospital cardiac arrest is still today a challenge for emergency medical services, hospitals, patient and just like in term of socio-economic costs and scientific challenge due to its high mortality rate and poor outcome.
Case Presentation: We present a case of prolonged mechanical cardiopulmonary resuscitation in a 37 years old man, found by the wife, gasping with a shockable ventricular fibrillation at the first contact with paramedics, which was nevertheless not considered eligible to extra-corporeal life support due to the not witnessed cardiac arrest. The patient did not have any neurological nor cardiac disabilities.
Conclusion: We report this successful case of prolonged mechanical cardiopulmonary resuscitation with a good neurological outcome even if not eligible to extra-corporeal life support due to poor expected outcome, in order to highlight the need of further investigations about the role of ECMO in the cardiac arrest setting, thinking about which patient’s feature could be considered a predictors of a positive response to an invasive cardiopulmonary support.
Introduction
Out of hospital cardiac arrest (OOHCA) is, despite progresses in advanced cardiac life support (ACLS) protocols (1), still today graved by high mortality rate in large cohorts studies, as shown by Gasner. [2] Extracorporeal Membrane Oxygenation (ECMO) is a useful treatment for refractory out-of-hospital cardiac arrest (OOHCA), and, as discussed by Lee et al.[3], it could be a valid instrument in the management of it. Reynolds et al. in a recent retrospective analysis of OOHCA demonstrated a decrease in the probability of survival and an hospital discharge with a good functional and neurological outcome within each minute of cardiopulmonary resuscitation.[4] Probability of good functional outcome after 15 minutes of CPR was down to 2%, when compared to 75% in patients resuscitated up to 10–15 minutes [2]. It is reported a rate of return on spontaneous circulation (ROSC) more than 90% in patients resuscitated for less than 10 minutes, compared to 50% when the cardiopulmonary resuscitation (CPR) duration was over 30 minutes [3]. Today, despite efforts in public access defibrillation and early CPR programs, ROSC in OOHA is below 10% [4] Although differences in Emergency Medical Service (EMS) structures and CPR practices, a variability of ROSC in the range of 10.0-50.0%, and hospital survival from less than 5.0% to 30.0% has been registered in a large European study [5].
Case Presentation
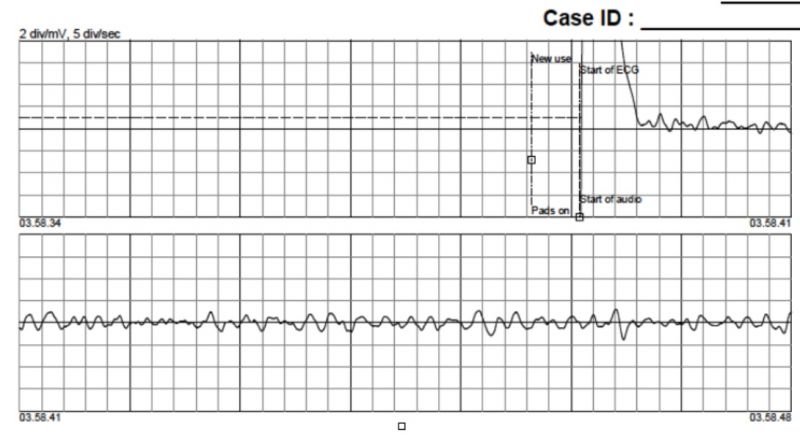
We present a case of successful CPR in a 37 years old male patient. He was found in cardiac arrest (CA) by the wife, who was awaked by her “unresponsive husband, who was strongly snoring”, as she reported to the emergency dispatcher at 112 emergency call at 03:54 am. Cardiopulmonary resuscitation was started by phone order, and a bystander neighbour assisted the patient on scene (03:56 am). An advanced life support team and a basic life support (BLS) ambulance were simultaneously dispatched, with the latter reaching the patient at 04:03 am, with cardiac arrest confirming (figure a), starting resuscitative manoeuvres, and reporting that a shockable rhythm was immediately discharged by the automated external defibrillator (AED).
Figure a.Presentation rhythm recorded by AED
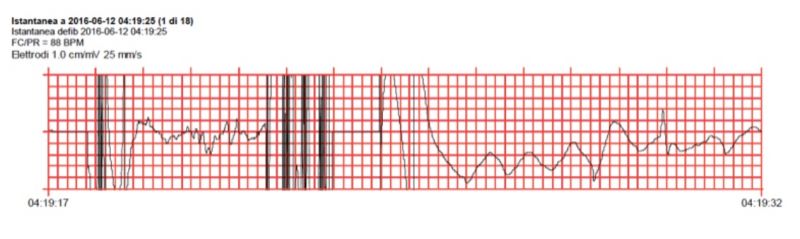
The ALS team was on the scene at 04:08, meanwhile a second AED shock was delivered without restoring a spontaneous circulation. Patient was immediately intubated and monitored by the medical doctor while the mechanical chest compression device was positioned and activated, a venous access was placed, epinephrine was administered intravenously, and mechanical CPR was simultaneously started by 04:10 am. End tidal expiration carbon dioxide monitoring showed a 11mmHg value while chest compressions. Monitor showed a coarse ventricular fibrillation (VF) at third analysis, as showed in figure [b]; another shock was attempted and antiarrhythmic drug bolus was administered. Despite the bolus, a persistent VF rhythm was registered and MgSO4 bolus was administered.
Figure b. Presentation rhythm on ALS provider Monitor
Very quickly pupil examination demonstrated equal, isochoric, miotic pupils.
With a few more questions, emerged that patient did not suffer any past medical problem, did not have any fever, headache or illness in the last 24 hours before cardiac arrest.
At this time, after 14 minutes, ACLS team leader requested authorization for medical evacuation to an ECMO center, with ACLS manoeuvres in the meantime.
While preparing the patient for transportation (a narrow flight of stairs had to be negotiated) the referring ECMO Hospital refused to accept the patient due to prolonged and invasive support, because of “uncertainty about the patient no flowing state”.
Ambulance with the advanced medical team leaved the scene, with the patient under CPR, at 04:38AM and was diverted to the nearest hospital which had an Intensive Cardiac Unit, an hemodynamic capability, thoracic and vascular surgery, but without any cardiac surgery possibilities.
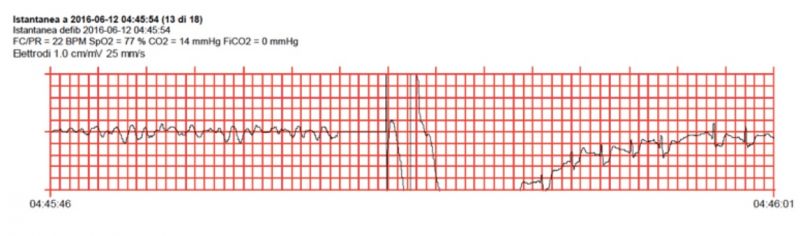
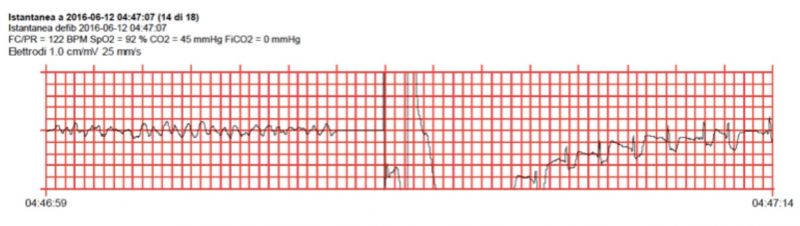
During patient transportation, a total number of four more DC shocks were delivered obtaining a first temporary ROSC at 04:43 am, followed by a shocked VF (figure c) that brought to a definitive ROSC at 04:46 am (figure d).
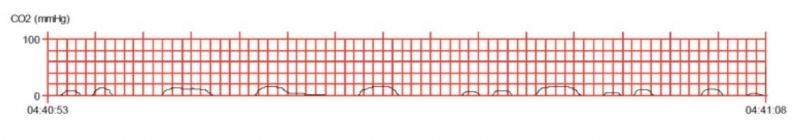
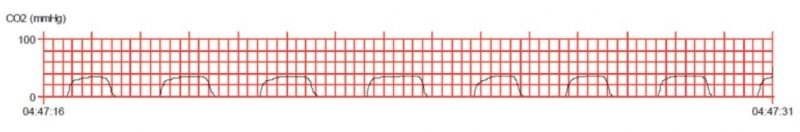
At this time, two minutes of CPR showed a steep rise in ET-CO2 up to 46mmHg (figure e-f). An atrial fibrillation was observed and a 12 leads EKG did not demonstrate any STEMI/NSTEMI.
A basal CT scan of the brain did not show any intracranial bleeding. Chest and abdomen were normal.
A subsequent cerebral RMN, after 24 hours, did not show any sign of cerebral ischemia. Neurological physical examination was unremarkable. The neurological outcome, using Cerebral Performance Category (CPC), one month after cardiac arrest was 1 (good cerebral performance)
He was subsequently studied by cardiologists, and a cardiac defibrillator was implanted (ICD).
The patient was discharged from the hospital without any neurological deficit, and at the time (December 2017) is conducting a normal life.
Interestingly, the employers has been so much impressed by this episode that decided spontaneously to deliver an AED program to all employees and customers.
Discussion
Historically, from the first extracorporeal successful cardiopulmonary support in 1953, when Professor Gibbon indication to extracorporeal life support was to sustain open heart surgery, today with miniaturisation of devices, improvement of technology, ECLS could be started successfully even in “Spoke” hospitals with percutaneous techniques with proper training and dedicated equipe. Guidelines have been written, but at the time inclusion criteria are not totally uniform. Extracorporeal Life Support Organisation, in December 2013, published guidelines for ECPR cases, writing that AHA guidelines for CPR recommends consideration of ECMO to aid cardiopulmonary resuscitation in patients who have an easily reversible event and have had excellent CPR. Instead, all contraindications to ECMO use (such as Gestational age < 34 weeks) should apply to ECPR patients. ELSO considered such a futility the cases in which unsuccessful CPR (no return of spontaneous circulation) for 5-30 minutes is performed, without considering the “time of no flow” before resuscitation providers arrival; however ECPR may be indicated on prolonged CPR if good perfusion and metabolic support is documented. [7].
Lazzeri et al. in their paperwork included all patients with an estimated interval of less than 15 minutes from the time of collapse to CPR start with or without witnessed CA, independently of rhythm of presentation. [8]
This case demonstrates how patients who present a shockable rhythm at the first contact (BLS or ALS team, independently), despite an not-witnessed “no flow time”, and who have recurrent cardiac arrest after the first ROSC, shall be always addressed to the nearest ECMO center, if logistically suitable. This observation is even more appropriate considering patients under 40 years without comorbidities. In fact there was a statistically significant reduction in the probability of survival to hospital discharge with increasing numbers of chronic conditions, such as congestive heart failure, prior myocardial infarction, hypertension, and diabetes (OR 0.84 for each additional chronic condition). The impact of comorbidities was more prominent with longer EMS response intervals. Furthermore inherited electrophysiological abnormalities, termed primary electrical diseases, are increasingly common in patients under 40 years without comorbidities .These conditions including Wolff-Parkinson White syndrome, long QT syndrome, Brugada syndrome and catecholaminergic polymorphic ventricular tachycardia (CPVT) are associated with a better outcome also after a prolonged CPR. (11)(12)
Interestingly, this patient had a probability of survival, at one month, of 68%, if considering only the initial rhythm (VF), but the dynamic probability to survive with a good cerebral function after 30 minutes of CPR is below 0,4% as demonstrated by Yoshikazu in a recent paperwork. In the same paper the authors demonstrated no survivors at 53 minutes of CPR. (13)
In this contest, it is especially important to have a defined ECMO center protocol: firstly in order to permit the support of the circulation and tissue perfusion if there is not any ROSC in the hospital, while appropriate treatment are being performed; secondly ECMO could assist the left ventricular function in case of a cardiogenic shock after ROSC.
Today, no clinical studies on ECPR are in literature and published series available have used strict criteria of inclusion and exclusion for patient selection for ECPR .
Although these inclusion criteria are highly variable, most of them only included patients aged between 18 and 75 years with comorbidity limited in circulatory arrest from cardiac origin, after traditional CPR for more than 10 minutes without ROSC. These inclusion criteria must be taken into account in the selection by the operator of potential candidates to ECPR. [9]
ECPR, as mentioned in the latest AHA guidelines on CPR and ECC, can be considered an alternative to the traditional CPR for cardiac arrest in selected patients and for which the suspected etiology of cardiac arrest is potentially reversible. [9]
Conclusions
Inclusion criteria hypothesis of which range for “unwitnessed” could be acceptable “ex ante”, especially in young patients, should be carefully weighted by further studies. In our case a shockable rhythm was still present 14 minutes after first delivered shock attempted at BLS arrival and a VF was persistently present up to ROSC; the other point is that a wider diffusion of ECMO inclusion criteria should stress the transformation made to ACLS in the recent years; finally the “ECMO shopping” should be avoided by a prewritten prehospital-inhospital common protocol.
Acknowledgments
Authors retrieved CPR data with a commercially available USB pen drive from a X series Zoll defibrillator. Simple analysis was possible with free Zoll RescueNet Code Review softwareX}. Since, at the moment of this case, synchronisation between Autopulse and X series monitor was not possible, only basic CPR analysis was possible from monitor data. Authors do not have any commercial relation with Zoll and did not receive any fund for this research. [11]
References
- Guidelines ACLS , American Heart Association 2016
- Gräsner J-T, et al. A prospective one month analysis of out-of-hospital cardiac arrest outcomes in 27 countries in Europe. Resuscitation 68121-7 (2016).
- Lee et al., Out-of-hospital cardiac arrest patients treated with cardiopulmonary resuscitation using extracorporeal membrane oxygenation: focus on survival rate and neurologic outcome Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine (2016) 24:74.
- Reynolds J. C. et al., Duration of resuscitation efforts and functional outcome after out-of-hospital cardiac arrest: when should we change to novel therapies? 2013;128(23):2488–2494.
- Ornato J.P. et al., The Public Access Defibrillation (PAD) trial: study design and rationale. Resuscitation. 2003;56(2):135–147. doi: 10.1016/S0300-9572(02)00442-2. Shih C.-L., Lu T.-C., Jerng J.-S., et al. A web-based Utstein style registry system of in-hospital cardiopulmonary resuscitation in Taiwan. Resuscitation. 2007;72(3):394–403. doi: 10.1016/j.resuscitation.2006.07.020.
- Kim et al., An optimal transition time to extracorporeal cardiopulmonary resuscitation for predicting good neurological outcome in patients with out-of-hospital cardiac arrest: a propensity-matched study. Critical Care 2014, 18:535
- ELSO ECPR Supplement to the ELSO general guidelines, December 2013, version 1.3 Pag.
- Lazzeri C. et al., Extracorporeal life support for out-of-hospital cardiac arrest: Part of a treatment bundle. European Heart Journal, Acute Cardiovascular Care, 2015 May 12.
- American Heart Association, Guidelines 2015 on CPR and ECC.
- Poppe M. et al., The incidence of “load&go” out-of-hospital cardiac arrest candidates for emergency department utilisation of emergency extracorporeal life support: A one-year review. Resuscitation 91 (2015) 131–136
- RescueNet Software, at: http://www.zoll.com/medical-products/data-management/rescue-net-fire-ems/code-review
- Carew Ht et al., Chronic health conditions and survival after out-of-hospital ventricular fibrillation cardiac arrest. Heart 2007; 93:728
- Yoshikazu Goto et al. Relationship between the duration of cardiopulmonary resuscitation and favorable neurological outcomes after out of hospital cardiac arrest; A prospective, nationwide, population based color study. J Am Heart Assoc. 2016;5:e002819 doi: 10.1161/JAHA. 115002819